Benzodiazepines (BZDs) are among the most commonly prescribed drugs in the U.S. Data for 1996-2013 show a 67% increase in adults filling BZD prescriptions. During the same period, the total quantity of BZDs filled increased 3.3-fold and overdose mortality involving BZDs increased 5.3-fold. An estimated 75% of deaths involve the use of opioids in addition to BZDs (2), likely due to worsening of opioid-induced respiratory depression by BZDs. Compounding these concerns are the use of non-Food and Drug Administration (FDA)-approved BZDs.
BZDs in the U.S. fall into essentially two groups: FDA-approved and non-FDA-approved compounds (Figure 1). Non-FDA-approved BZDs can be delineated into two further groups: BZDs approved in other countries and designer BZDs (DBZDs) (often called synthetic, novel, or novel psychoactive substances).
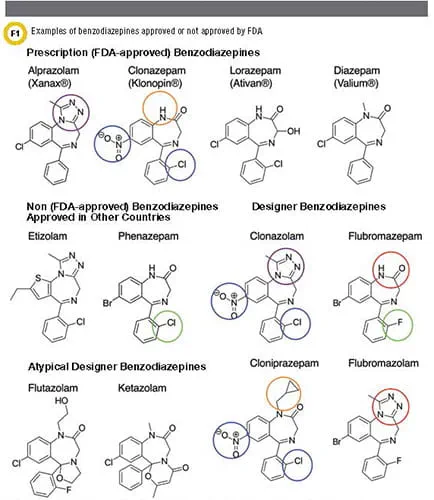
The latter can be further divided into BZDs prescribed outside the U.S. and true designer BZDs (DBZDs) not approved for medical use anywhere in the world. DBZDs are often structurally very similar to approved BZDs (exceptions are flutazolam and ketazolam). A few examples follow. Cloniprazepam is metabolized into clonazepam by the removal of the cyclopropylmethyl group (circled in orange). Clonazolam can be considered a hybrid of clonazepam (functional groups circled in blue) and alprazolam (triazolo group circled in purple). Similarly, flubromazolam is a triazolo analog of flubromazepam (difference circled in red). Flubromazepam only differs from phenazepam by the substitution of the chlorine group by fluorine (circled in green). Adapted from Marin et al. (7) with permission from AACC.
Several BZDs, such as etizolam and phenazepam, are approved in a handful of countries but are often misused in the U.S. and other countries. Etizolam was first introduced in Japan and is also approved in India and Italy. Phenazepam was developed in the Soviet Union and is still approved for use in Russia and other former Soviet states. DBZDs have often been described in the scientific or patent literature as compounds that were explored by pharmaceutical companies but never developed into drugs (3). They are not approved for medical use anywhere in the world.
Chemically, non-FDA-approved BZDs maintain much of the primary structure of FDA-approved BZDs. However, they are modified from this primary structure by the addition and/or deletion of certain functional groups. Some DBZDs are hybrid molecules of different FDA-approved BZDs. They may also be either potent metabolites of FDA-approved BZDs or compounds metabolized into FDA-approved BZDs. For example, the DBZD clonazolam may be considered a hybrid of alprazolam (technically a triazolo BZD) and clonazepam, both of which are commonly prescribed BZDs. A newer abused DBZD, flualprazolam, is based on alprazolam with an additional fluorine group. These additions and substitutions at specific locations have generally predictable effects on BZD activity (Figure 2).
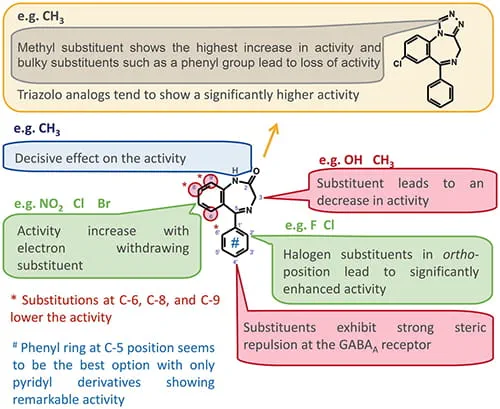
General structure-function association for different benzodiazepine modifications. Reproduced from Moosmann et al. (3) with permission from Springer International Publishing.
Trends and Public Health Concerns
Today, many non-FDA-approved BZDs are sold via illicit marketplaces such as the darknet (also called dark web or deep web), a part of the internet that is not indexed and can only be accessed using special browsers. They’re also sold on other obscure websites that label these compounds as research chemicals or legal alternatives. This is concerning as data are limited on the clinical effects and pharmacologic characteristics of DBZDs.
One recent study retrospectively evaluated multiple case reports and found that the clinical effects of DBZDs and etizolam were generally consistent with sedative-hypnotic toxidrome, as would be expected for BZD derivatives. Severe effects, however, were uncommon (4). Thus, clinically suspecting non-FDA-approved BZD use may prove itself difficult because there seems to be no distinct difference from the sedative-hypnotic toxidrome seen in FDA-approved BZDs. Further, many of the cases in which non-FDA-approved BZDs have been detected were in conjunction with other classes of commonly abused drugs, such as opioids (4-6). It is important to note, however, that single agent exposures of non-FDA-approved BZDs are on the rise (4).
Illicit markets often sell non-FDA-approved BZDs under the guise of FDA-approved BZD names (6,7). For example, flubromazolam and etizolam have been detected in fake Xanax tablets instead of alprazolam (3,8). As the pharmacological effects of these compounds are largely unknown, this trend poses dangers not only for recreational users who believe they are purchasing a familiar BZD, but also potentially for unwary patients.
The latter group may not be at risk as an unintended side effect of a potential restriction on BZDs, which in general have the risk for physical dependence and addiction. A clamp down on BZD prescribing could lead to patients seeking these medications through illicit channels. This concept is not new and parallels the ongoing U.S. opioid crisis.
Current Monitoring Methods and Their Limitations
Most data on reported exposures and trends of non-FDA-approved BZD use in the U.S. are reported retrospectively by large institutions such as the National Poison Data System and the Drug Enforcement Administration. Internationally, early warning systems exist through the United Nations Office on Drugs and Crime and the European Monitoring Centre for Drugs and Drug Addiction.
The U.S. does not have a regularly used, centralized reporting system, and real-time monitoring is often lacking. However, even efforts that capture information more prospectively, such as the STRIDA project in Sweden, still underestimate the total number of DBZD-related intoxications (5). Thus, usage and outbreaks are often underreported and not well defined until communities begin to experience their effects. Notably, once a DBZD has been regulated as a controlled substance, often one or more new (non-regulated) DBZDs make their way into a community (3) (Figure 3). This continues to be a legal game of whack-a-mole in which regulatory and enforcement agencies, monitoring institutions, clinical laboratories, and healthcare providers are always playing catch-up with drug outbreaks.
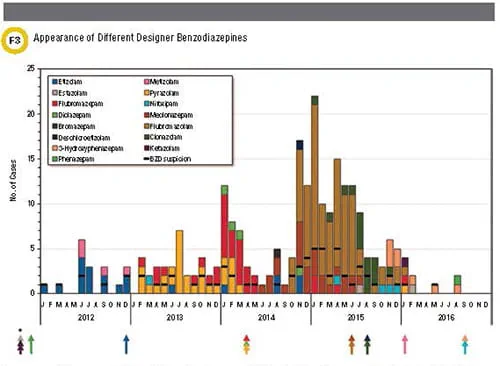
Appearance and disappearance of different designer benzodiazepines (DBZDs) and etizolam/phenazepam in Sweden during 2012-2016 analyzed as part of the STRIDA project. Disappearance of a DBZD often coincides with the time of controlled substance classification (represented by the arrows). As indicated by the asterisk, some compounds were classified before 2012. Reproduced from Bäckberg et al. (5) with permission from Taylor & Francis.
Suggestions to Improve Monitoring
In order to improve monitoring of non-FDA-approved BZDs, a few concepts are essential. First, monitoring should occur in real time through a centralized reporting system. Centralized, free-of-charge testing for providers who suspect designer drug use is likely a valuable adjunct. Such testing was successfully implemented in the STRIDA project.
In addition, this information should be continuously updated. Making a real-time database useful requires a standardized way of continually disseminating the information, reaching not only toxicological and laboratory experts but also interested health providers. A local, real-time heatmap of identified DBZDs and designer drugs in general would provide invaluable data to providers and laboratorians.
Finally, monitoring should be proactive. That is, can we predict which novel DBZDs will appear next within a community or location? For example, could we take selected data from patents, scientific literature on BZDs that were never developed into drugs, current data on approved and non-approved BZDs, timelines of newly identified DBZDs in communities, and integrate this information to make predictions, potentially through the use of artificial intelligence?
For example, a current trend is to produce triazolo analogs of FDA-approved BZDs or DZBDs: clonazolam is the triazolo analog of the FDA-approved clonazepam and flubromazolam is the triazolo analog of flubromazepam, a DBZD (Figure 1). Another trend is to produce various modifications of etizolam (3).
Monitoring could also take the shape of gathering data from social media where DBZDs are discussed, such as Reddit and Bluelight, as well as tracking items for sale on obscure internet sites and the dark web.
In aggregate, standards of potential new DBZDs could be produced proactively, not unlike the Psychoactive Surveillance Consortium and Analysis Network project for surveillance of synthetic cannabinoids (9). These compounds could then be added to confirmation assays ideally before, or soon after, the start of an outbreak. A comprehensive, proactive approach would enhance preparedness and detection both on a clinical and laboratory level.
Challenges in Identification and Interpretation
The good news is that immunoassays for BZDs generally have good cross-reactivity for non-FDA-approved BZDs (1,10). The exceptions are DBZDs with atypical structures such as flutazolam and ketazolam (Figure 1). However, as these cross-reactivity studies generally test parent compounds, it is possible that primary drug metabolites might not cross-react using antibody-based assays. This problem has been suspected in the case of flubromazepam (7).
However, when a preliminary positive sample that contains a non-FDA-approved BZD is analyzed for confirmation by mass spectrometry (MS), it will likely be negative, as many targeted BZD confirmation assays do not test for these compounds. This may lead to the incorrect interpretation of a false positive immunoassay-based BZD result. A study in Sweden found that 40% of presumably false-positive BZD results actually contained a non-approved BZD (7).
Due to the rapidly changing landscape of DBZDs, clinical and forensic toxicology laboratories face an almost impossible task to keep their targeted methods up to date. Clinical laboratories have the option of using untargeted data acquisition by high-resolution MS, for example using a quadrupole-time-of-flight (QTOF) instrument. This approach offers fast method development, and novel DBZDs can be preliminarily identified based on the highly accurate exact mass and isotope pattern and later confirmed with a reference standard. Additionally, a laboratory could analyze data retrospectively for compounds that were not in the library during the time of analysis. However, high-resolution instruments remain costly.
Another challenge for analytical identification—especially in urine—is the limited knowledge of DBZD metabolites. In vitro human liver microsome-based and single-subject self-administration studies have shed some light on which metabolites are likely targets for detection. Targeting the parent compound may be sufficient to detect some DBZDs. For example, pyrazolam is mainly excreted as unchanged parent drug. However, for other DBZDs, only metabolites may be detectable in urine. For example, < 0.5% of etizolam is excreted as unchanged parent drug (7). Moreover, such studies lag behind the first reported use of the novel DBZD.
Lastly, as new DBZDs appear quickly, there is a considerable lag time in the availability of reference standards. As mentioned above, predicting novel DBZDs and proactive synthesis of standards would help circumvent several of the aforementioned limitations.
In addition to incorrectly interpreting positive immunoassay results with negative confirmations, clinical laboratorians must navigate other pitfalls in interpreting MS results (3). For example the metabolite of the DBZD cloniprazepam is the FDA-approved drug clonazepam (Figure 1); thus, one could falsely interpret the use of cloniprazepam as clonazepam use. Similarly, the metabolites of diclazepam are the pharmaceutical drugs delorazepam, lormetazepam, and lorazepam (although only lorazepam is FDA-approved) (7).
Conclusion
The ever-evolving landscape of DBZDs remains a challenge for the public health sector, as well as healthcare providers and clinical and forensic laboratorians. To stay current on the latest trends in DBZD use laboratorians should familiarize themselves with both the currently available resources used for monitoring and early warning systems.
Although challenging, laboratories should do their best to keep an updated list of relevant DBZDs in their MS confirmation assays and consider whether these DBZDs will be detected on their specific immunoassay platforms. High-resolution MS systems are helpful tools to keep up with quickly appearing (and disappearing) DBZDs.
Lastly, laboratorians must collaborate with medical toxicologists, emergency department physicians, and other providers to ensure appropriate support and education to treat patients who present with a clinical suspicion of DBZD abuse.
Maximo J. Marin, MD, is an assistant professor in the Department of Pathology and Laboratory Medicine at the Keck School of Medicine of the University of Southern California in Los Angeles and director of clinical chemistry for Keck Medical Center, Los Angeles. +Email: [email protected]
Xander M. R. van Wijk, PhD, DABCC, is an assistant professor in the Department of Pathology at the University of Chicago Pritzker School of Medicine and assistant director of clinical chemistry laboratories for UChicago Medicine. +Email: [email protected]
References
- van Wijk XMR, Yun C, Hooshfar S, et al. A liquid-chromatography high-resolution mass spectrometry method for non-FDA approved benzodiazepines. J Anal Toxicol 2019;43:316-20.
- Bachhuber MA, Hennessy S, Cunningham CO, et al. Increasing benzodiazepine prescriptions and overdose mortality in the United States, 1996-2013. Am J Public Health 2016;106:686-8.
- Moosmann B, Auwarter V. Designer benzodiazepines: Another class of new psychoactive substances. Handb Exp Pharmacol 2018;252:383-410.
- Carpenter JE, Murray BP, Dunkley C, et al. Designer benzodiazepines: A report of exposures recorded in the national poison data system, 2014-2017. Clin Toxicol (Phila) 2019;57:282-6.
- Backberg M, Pettersson Bergstrand M, Beck O, et al. Occurrence and time course of NPS benzodiazepines in Sweden - results from intoxication cases in the STRIDA project. Clin Toxicol (Phila) 2019;57:203-12.
- Zawilska JB, Wojcieszak J. An expanding world of new psychoactive substances-designer benzodiazepines. Neurotoxicology 2019;73:8-16.
- Marin MJ, van Wijk XMR. Designer benzodiazepines: New drugs challenge laboratories. Clinical and Forensic Toxicology News (Quarterly, AACC/CAP) June 2018:1-6.
- Arens AM, van Wijk XM, Vo KT, et al. Adverse effects from counterfeit alprazolam tablets. JAMA Intern Med 2016;176:1554-5.
- Gerona R. The utility of LC-QTOF/MS in proactive synthetic cannabinoid testing in the psychoactives surveillance consortium and analysis network (P SCAN) [Abstract]. MSACL 2018.
- Pettersson Bergstrand M, Helander A, Hansson T, et al. Detectability of designer benzodiazepines in CEDIA, EMIT II Plus, HEIA, and KIMS II immunochemical screening assays. Drug Test Anal 2017;9:640-5.
